Number of people on waiting lists for non-urgent hospital treatment in Wales hits record levels
The number of people on waiting lists for non-urgent hospital treatment in Wales have again hit record levels.
The number of people waiting in June 2021 was 2.9% higher (17,869 more patient pathways waiting) than in the previous month and 36.5% higher than in the same month before the pandemic.
Data shows in North Wales in June there were 131,362 people waiting to start treatment, again the highest since records begin 10 years ago – with over 51,000 waiting over 36 weeks.
Emergency departments also saw increased demand during July with over 94,000 patients attending.

Average time spent in emergency departments remain at the longest since comparable data was first collected in April 2012.
At the Wrexham Maleor Hospital figures show that 53.9 per cent of those who attended spent less than four hours in A&E.
72.2 per cent were seen within eight hours and 83.7 per cent within 12 hours.
“We also saw the largest number of specialist consultations completed and treatments started in any month since the start of the pandemic.”
“The total number of patients starting their first cancer treatment and the number of patients starting treatment within the target time were the second highest since the current records began.”
“Today we announced a further £140m to help NHS Wales tackle the treatment backlog built up during the Covid pandemic. This is on top of the initial £100m announced in May.”
“Pressures on our emergency services are also growing. The ambulance service received more calls last month than in any month since the pandemic began. Attendance at emergency departments was also the highest since the start of the pandemic.”
“We encourage people to consider the best options for care, and not necessarily head to their local emergency department. To get the right care, first time people can also use the online 111 service and their local pharmacist where appropriate.”
“Last month the Health Minister announced plans to transform the delivery of urgent and emergency care, supported by £25m a year. We are working with health boards to deliver these plans well ahead of winter.”
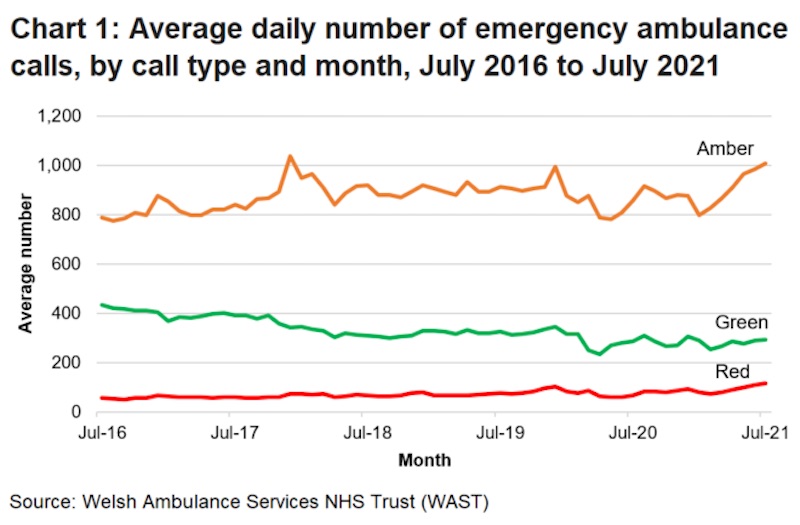
Last month saw the highest daily average number of calls made to the Welsh Ambulance Service recorded since the pandemic began; this is also the third highest daily average total calls since comparable data was first collected in October 2015.
The trust was forced to declare a ‘Business Continuity Incident’ in July due to increased demand on its services.
A business continuity incident is an event or occurrence that disrupts, or might disrupt, an organisation’s normal service delivery, below acceptable predefined levels, where special arrangements are required to be implemented until services can return to an acceptable level.
Of the calls made a record high percentage (8.2 per cent) of calls to the ambulance service were recorded as immediately life threatening (red calls) since comparable data was first available in May 2019.
July also saw the second highest daily average number of amber calls made to the ambulance service since comparable data was first collected in October 2015.
Commenting on the figures, Welsh Conservative Shadow Health Minister, Russell George MS, said:
“Even before the pandemic, we were used to seeing some devastating numbers on healthcare in Wales due to Labour mismanagement. But to record the worst ever A&E waiting times and the longest NHS treatment waiting list in the same month shows a complete lack of leadership.
“Given how catastrophic these numbers are, it makes you wonder how many years before we can expect to get close to breaking all the right records rather than all the wrong ones.
“Although we know August is a difficult month for A&E, now that we are well past Covid peaks, we should be seeing improvements in meeting the needs of patients. We are seeing this in England but sadly not in Wales, something that is simply not acceptable.
“The funding announced to tackle the backlogs is a start and hopefully will be directed towards our calls for filling the 3,000 NHS staff vacancies, expanding the use of rapid diagnostic centres, and exploring the introduction of specialist hubs to tackle routine surgery as soon as possible.
Spotted something? Got a story? Email: [email protected]
Latest News
